Many believe that having more coils in an IUD makes it more effective, but this is a myth. Effectiveness depends on proper design, placement, and quality, not coil count. The key factors are how well the device fits your uterus and correct insertion by a healthcare professional. Coil count alone doesn’t determine protection. To understand why device quality and proper fit matter more, keep exploring this topic further.
What Is an IUD and How Does It Work?
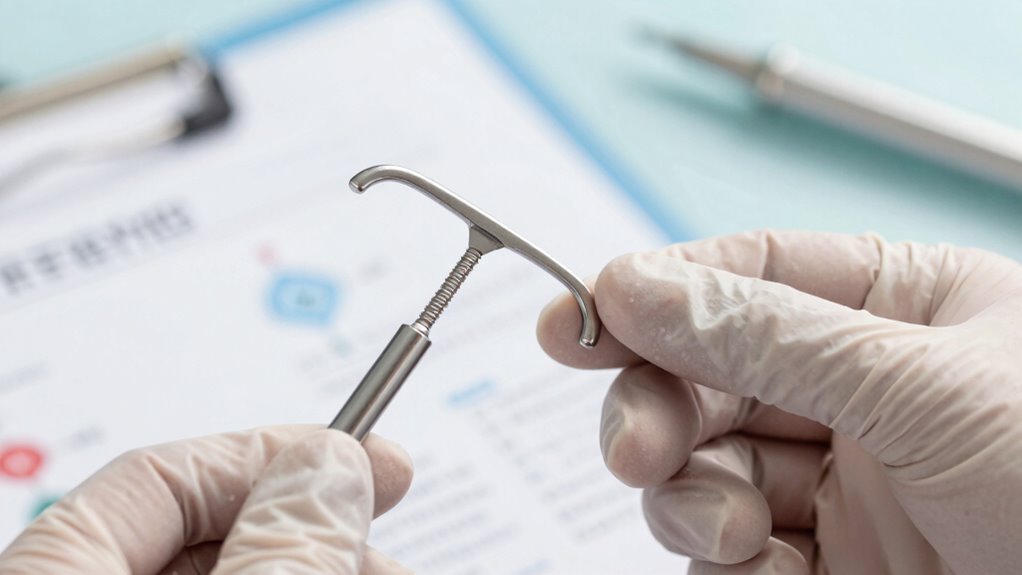
An intrauterine device (IUD) is a small, T-shaped contraceptive inserted into your uterus to prevent pregnancy. Many coil myths surround IUDs, but their effectiveness depends on several factors, including correct placement and type. IUDs work mainly by preventing fertilization or implantation, making them highly reliable when used properly. You might hear that IUDs are only effective for some women or that they cause health issues, but research shows they have a success rate of over 99%. The effectiveness factors include proper insertion and regular check-ups. Understanding how an IUD works helps dispel myths and highlights its reliability. Remember, the number of coils or the type doesn’t determine effectiveness—proper use and professional placement do. Additionally, contraceptive technology continues to advance, enhancing the safety and efficacy of devices like IUDs.

Any Size Copper Tube Copper Coil Roll Soft Coil Pack Of 16.4Foot Length (6 * 1.5mm)
Durable Copper Material: Crafted from high-quality copper, this tube coil roll ensures long-lasting performance and resistance to corrosion.
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
What Are Common Myths About Coil Count and Effectiveness?

Many people believe that the number of coils in an IUD directly affects its effectiveness, but this is a common myth. Coil myths often lead to misconceptions about how IUDs work, causing unnecessary confusion. The truth is, effectiveness isn’t determined by coil count but by the device’s design and hormone or copper content. Here’s a quick comparison:
| Coil Count | Effectiveness Myth | Reality |
|---|---|---|
| More coils | Increases effectiveness | Coil count doesn’t matter |
| Fewer coils | Less effective | Effectiveness depends on type |
| High coil count | Better protection | Not supported by evidence |
| Low coil count | Less reliable | Effectiveness misconception |
Understanding these coil myths helps you make informed choices about your contraception. Additionally, advancements in cloud technology are transforming healthcare data management, emphasizing the importance of accurate information and reliable devices.

Opill, Daily Birth Control Pills, Over-the-Counter Progestin-Only Oral Contraceptive, FDA-Approved & Estrogen-Free, 28 Count
OTC BIRTH CONTROL PILL: Opill is the first over the counter, daily oral contraceptive pill that is available…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
How Do Copper and Hormonal IUDs Differ?

Copper and hormonal IUDs differ mainly in their materials and how they prevent pregnancy. You’ll find that hormonal IUDs release hormones, while copper ones rely on the metal’s properties. Understanding these differences helps you choose the right option for your needs. Additionally, affiliate disclosure ensures transparency when considering purchasing options related to IUDs. The halal status of these devices is not typically a concern, but it’s important to consult healthcare providers for personalized advice. Recognizing AI-driven medical innovations can also inform your decision-making process about contraceptive methods. Proper piercing care and hygiene practices are essential to prevent infections, which is important for overall reproductive health.
Material Differences and Effectiveness
While both copper and hormonal IUDs serve as effective long-term birth control options, they differ markedly in their materials and how they work. Copper IUDs are made from a plastic frame wrapped with copper wire, which creates a toxic environment for sperm. They boast high coil durability, meaning they can last up to 10 years without degradation. Hormonal IUDs contain a small amount of progestin, encased in a plastic or polyethylene frame, releasing hormones gradually. This design emphasizes material safety, as the hormones are localized, reducing systemic effects. The materials used in each IUD type influence their effectiveness and side effects, but both are proven reliable. Your choice depends on personal health considerations, preferences, and how your body responds to their material composition. Material composition plays a crucial role in how each IUD interacts with your body and potential side effects.
Hormonal vs. Non-Hormonal
Hormonal and non-hormonal IUDs differ primarily in how they prevent pregnancy. Hormonal IUDs release progestin, which thickens cervical mucus and suppresses ovulation, leading to hormonal effects that can lighten periods or cause spotting. Non-hormonal copper IUDs create an inflammatory response toxic to sperm, with no hormonal interactions involved. Here’s a quick comparison:
| Feature | Hormonal IUD | Non-Hormonal Copper IUD |
|---|---|---|
| Primary mechanism | Hormonal effects, ovulation suppression | Copper-induced sperm toxicity |
| Hormonal interactions | Releases progestin | No hormones involved |
| Typical side effects | Irregular bleeding, hormonal symptoms | Heavier periods possible |
| Duration | 3-7 years | 10-12 years |
| Suitability | Hormonal sensitivities | Hormone-free preference |
Additionally, understanding the mechanisms of action can help individuals choose the most suitable option for their health needs.

SimCoach Intrauterine Device Training Kit, IUD Training Model, Female Intrauterine Contraceptive Device Simulator Trainer
TRAINING IUD MODEL FOR MEDICAL PRACTICE: The IUD training model is made from plastic material, odorless, and non-toxic….
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Why Coil Count Isn’t a Reliable Measure of Protection?

A higher coil count doesn’t automatically mean better protection because material quality and design play vital roles. If the coil isn’t well-made or properly fitted, it can compromise effectiveness regardless of how many coils there are. So, focusing on quality and fit is more important than just counting coils.
Material Quality Matters
Coil count alone doesn’t guarantee your mattress’s protection because the quality of the materials used is just as important. High coil counts with low-quality materials can be less durable and supportive. Material quality affects comfort, longevity, and overall protection. Even a mattress with fewer coils can outperform a high-coil model if it uses superior materials.
| Material Type | Impact on Protection |
|---|---|
| High-Quality Foam | Adds durability and comfort |
| Premium Fabric | Enhances breathability and feel |
| Stronger Springs | Improves support and longevity |
Focusing solely on coil count ignores these vital factors. Material quality determines how well your mattress performs over time.
Design and Fit
While a higher coil count might suggest better protection, it doesn’t guarantee a perfect fit or ideal design. The quality of coil design matters more; a well-designed coil ensures even coverage and proper support. Even with many coils, if the mattress or pillow doesn’t fit your body correctly, you won’t get the protection you need. Fit assessment is vital—look for how well the product contours to your shape and supports your pressure points. An ideal fit reduces gaps and pressure points, regardless of coil count. Remember, the goal isn’t just more coils but better coil placement and design that match your body’s needs. Focus on fit and coil design to guarantee comfort and protection, rather than relying solely on coil count. For optimal protection, choosing products with advanced coil technology can make a significant difference in performance. Additionally, paying attention to natural materials used in the construction can enhance durability and comfort. Moreover, understanding coil placement patterns can help ensure even support and reduce pressure points. Incorporating ergonomic design principles can further improve the overall efficacy of the sleep surface.
Best T-shaped IUD
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
How Are IUDs Designed? The Role of Coils in Functionality

Understanding how IUDs are designed reveals the essential role that coils play in their functionality. The coil design is carefully engineered to guarantee effective contraception while minimizing side effects. The shape, size, and placement of the coils influence how the device interacts with your uterus. Material innovation is key in creating coils that are both safe and durable, often involving biocompatible materials like copper or hormone-releasing components. These materials enhance the IUD’s ability to prevent pregnancy by creating a hostile environment for sperm or releasing hormones steadily. The precise design of the coils ensures the IUD stays securely in place and functions reliably over time. So, while the number of coils may vary, it’s the thoughtful design and innovative materials that truly determine how well your IUD works.
What Factors Really Impact IUD Effectiveness and Comfort?
Your IUD’s effectiveness and comfort depend on proper placement, so trusting your healthcare provider’s technique is vital. Your body size can influence how comfortable you feel with your IUD, and individual hormonal responses may affect side effects. Understanding these factors helps you make informed choices and manage your experience. Additionally, document management tools can help you keep track of your healthcare information and appointments to ensure proper follow-up. Ensuring proper IUD placement techniques can significantly impact both the effectiveness and comfort of your device. Proper placement techniques are essential for optimal outcomes and can reduce the risk of complications. Moreover, understanding the role of healthcare providers can help you advocate for proper procedure and care. Proper technique training for providers is crucial to ensure each patient receives the best possible outcome.
Proper Placement Techniques
Proper placement of an IUD is essential for maximizing its effectiveness and guaranteeing comfort. Your healthcare provider uses specific insertion techniques to position the coil correctly within your uterus, which is critical for peak performance. The coil design also influences placement; some IUDs are easier to position properly due to their shape or flexibility. Skilled insertion minimizes discomfort and reduces the risk of complications like displacement or perforation. During the procedure, your provider carefully measures uterine depth and angles to make certain the IUD sits in the right spot. Accurate placement not only enhances effectiveness but also decreases side effects. Trusting your provider’s technique and understanding the significance of proper positioning helps make sure your IUD works as intended and feels comfortable over time. Incorporating local automation can also assist providers in planning the procedure more precisely, further improving placement outcomes. Additionally, understanding the coil placement factors can help you discuss concerns and expectations with your healthcare provider.
Body Size Compatibility
Body size can influence both the comfort and effectiveness of an IUD, but it’s not the only factor that matters. Your body size, including uterine dimensions, can affect how well an IUD fits and feels. Smaller bodies may require a device with greater coil flexibility to guarantee proper placement and reduce discomfort. Coil flexibility allows the IUD to adapt to your unique anatomy, making insertion easier and improving comfort during use. Conversely, a less flexible coil might cause discomfort or even improper positioning if it doesn’t match your body’s size. It’s important to discuss your body size and anatomy with your healthcare provider. They can recommend the most suitable IUD type and design to maximize both effectiveness and comfort.
Individual Hormonal Responses
While coil count and size are important, individual hormonal responses play a significant role in how effective and comfortable an IUD feels. Your unique hormonal fluctuations can influence how your body reacts to the device, affecting both comfort and efficacy. Some people experience fewer side effects, while others may notice changes in mood, bleeding, or cramping due to their individual responses. Understanding these differences can help you choose the right IUD. Factors that impact your hormonal response include:
- Baseline hormone levels
- Lifestyle and stress
- Age and overall health
- Genetic predispositions
- Hormonal sensitivity
Recognizing that hormonal fluctuations vary among individuals helps explain why IUD experiences differ, regardless of coil count. Your body’s response is key to finding the most suitable option for you. Additionally, personalized care considering your unique hormonal profile can improve your experience with contraceptive methods. Hormonal fluctuations are influenced by multiple factors, making a tailored approach essential for optimal results. Furthermore, understanding the individual hormonal responses can help predict potential side effects and improve overall satisfaction with your chosen method.
Why Proper Insertion and Follow-Up Matter?
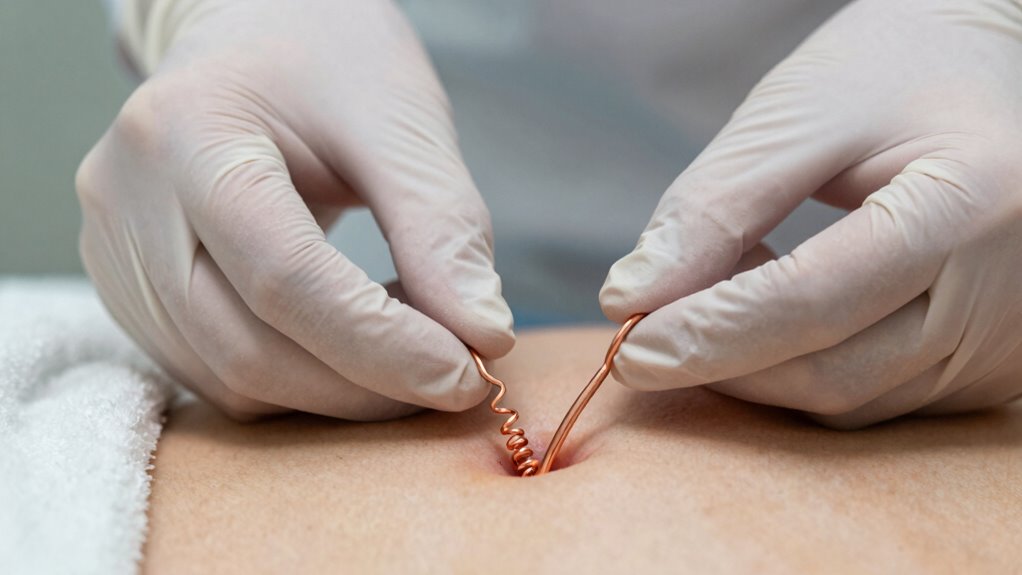
Inserting your intrauterine device (IUD) correctly is essential to guarantee it works effectively and minimizes potential complications. Proper insertion ensures the coil count is accurate and the device sits in the right position. This is critical for myth busting about IUDs, as many misconceptions stem from improper placement. Follow-up appointments allow your healthcare provider to verify the IUD’s position, check for any issues, and address concerns early. Regular medical monitoring is key to ensuring ongoing safety and effectiveness. Skipping these steps can lead to problems like displacement or discomfort, which could compromise effectiveness. Remember, the coil count alone doesn’t determine success; correct placement and ongoing monitoring are key. Understanding the affiliate disclosure and how it relates to medical products can help you make informed health decisions. Prioritizing proper insertion and regular follow-up helps ensure your IUD functions as intended, providing reliable contraception and peace of mind.
Do IUDs Affect Fertility After Removal? Myths and Facts

Many people worry that using an IUD might impact their future fertility, but the truth is that most women can conceive naturally after removal. IUDs don’t cause long-term fertility issues or damage your reproductive organs. Concerns about hormonal effects are common, but non-hormonal IUDs, like copper ones, have no hormonal influence. For hormonal IUDs, fertility preservation occurs quickly once the device is removed, and hormone levels return to normal. The myth that IUDs cause scarring or irreversible damage isn’t supported by research.
Most women can conceive naturally after IUD removal; it doesn’t cause long-term fertility issues.
Consider these facts:
- Fertility typically resumes within a month after removal
- No evidence links IUDs to infertility
- Hormonal effects are temporary and reversible
- IUDs do not impact ovarian reserve
- Most women conceive naturally after IUD removal
How Do Healthcare Providers Choose the Best IUD for You?
Healthcare providers select the most suitable IUD for you by carefully considering your individual health, lifestyle, and reproductive goals. They understand that coil count isn’t the only factor influencing effectiveness, and misconceptions about coil count can lead to unnecessary worry. Instead, they focus on the type of IUD—hormonal or copper—and how it fits your needs. Your provider evaluates your medical history, risk factors, and preferences to recommend an IUD that offers reliable protection and aligns with your life. They also consider factors like size, placement, and potential side effects. Remember, choosing the right IUD isn’t about coil count but about finding a device that matches your unique circumstances for safe, effective, and long-term contraception.
Why Focus on Quality and Fit Instead of Coil Count?

Focusing on quality and fit guarantees your IUD effectively meets your contraception needs while minimizing potential side effects. Instead of fixating on coil count, prioritize how well the IUD matches your anatomy and lifestyle. A properly fitted IUD ensures maximum effectiveness, regardless of coil number. When selecting an IUD, consider these factors:
- Comfort during insertion and wear
- Proper positioning within your uterus
- Your body’s response to the device
- Longevity and maintenance requirements
- Overall safety and reliability
High coil count doesn’t automatically mean better effectiveness. The best IUD for you depends on its quality, fit, and how well it aligns with your specific needs. Focus on these elements to ensure reliable contraception and minimize complications.
Frequently Asked Questions
Can IUDS Be Used as Emergency Contraception?
Yes, IUDs can be used as emergency contraception if inserted within five days after unprotected sex. The copper IUD is especially effective and considered very safe for emergency use. It’s a reliable option and provides long-term contraception afterward. If you need emergency options, consult your healthcare provider immediately to discuss IUD insertion and guarantee it’s the right choice for your safety and reproductive health.
How Long Does an IUD Typically Last Before Needing Replacement?
Did you know that most IUDs last between 3 to 10 years? Your IUD’s longevity depends on the type you have, but generally, you should plan for replacement around the 3 to 7-year mark. Regular check-ups help track its condition, ensuring effective contraception. When it’s time, your healthcare provider will recommend replacement timing to keep you protected and comfortable.
Are There Age Restrictions for Getting an IUD?
Age considerations typically don’t restrict your eligibility for an IUD, but your healthcare provider will evaluate your overall health and reproductive plans. Generally, women of reproductive age, including teenagers and those in their 40s, can get an IUD if they meet specific eligibility criteria. Your provider discusses your medical history and contraception needs to make certain of the best fit, regardless of age, making it a safe option for many women.
What Are the Common Side Effects After IUD Insertion?
You might experience some common side effects after IUD insertion, including hormonal side effects like mood swings, acne, or irregular bleeding, and insertion discomfort that may cause cramping or tenderness. While these symptoms can be bothersome, they often lessen within a few days. Remember, everyone’s experience varies, so stay attentive to your body’s signals and consult your healthcare provider if symptoms persist or worsen.
How Does Body Size Influence IUD Suitability?
Your body size can influence IUD suitability because body size considerations may affect IUD fit concerns. If you’re smaller or have a petite frame, your healthcare provider might assess whether a standard IUD will fit comfortably. Conversely, larger body sizes usually don’t pose significant issues. Ultimately, a professional evaluation helps determine the best IUD type and size for your body, ensuring effective contraception and comfort.
Conclusion
Remember, size isn’t everything—what truly matters is how your IUD fits your needs. Don’t get caught up in myths about coil count; focus on quality, proper placement, and your healthcare provider’s advice. As the saying goes, “It’s not the size of the dog in the fight, but the size of the fight in the dog.” Trust the process, stay informed, and choose what’s best for your health and peace of mind.









